The Ultimate Pet Care Glossary
Bordetella, commonly referred to as “Kennel Cough,” is a contagious upper respiratory illness in dogs. It spreads quickly through direct contact or airborne particles, making vaccination essential for dogs that come into contact with other dogs in places like neighborhoods, boarding facilities, daycare centers, dog parks, or groomers.
Puppies, young dogs, or those with weakened immune systems are more vulnerable and may experience more severe symptoms if not vaccinated.
Symptoms
- A dry, hacking cough
- A "honking" cough sound
- Nasal discharge
- Reduced appetite
- Lethargy
- Fever
Canine Influenza is a viral infection that emerged in 2012 from a mutated strain. Since it was a new virus, dogs exposed to it were highly susceptible to infection. A vaccine was developed to protect dogs and is available upon request. Fortunately, it is not contagious to humans.
Symptoms
- Nasal or eye discharge
- Coughing (can be either productive or non-productive)
- Difficulty breathing or rapid breathing
- Lethargy
- Vomiting
- Diarrhea
- Decreased appetite
Distemper is a highly contagious viral disease with no known cure, affecting dogs, cats, ferrets, and certain wildlife. The disease spreads through both direct and indirect contact.
Symptoms
- Unexplained weight loss
- Decreased energy levels
- Elevated body temperature
- Frequent vomiting
- Diarrhea
- Nasal congestion or discharge
The available vaccines are a combination of common, species-specific viruses.
For dogs, the vaccine protects against intestinal viruses such as Distemper, Hepatitis, Parainfluenza, and Parvovirus.
For cats, the vaccine guards against upper respiratory viruses, including Rhinotracheitis, Calicivirus, and Panleukopenia.
These vaccines are typically referred to as DHPP (for dogs) and FVRCP (for cats).
Puppies and kittens receive the distemper vaccine in a series, with annual boosters for young adults, and every three years for older pets and seniors.
Feline Leukemia (FeLV) is a viral infection transmitted between cats through saliva, feces, and during lactation. Nursing kittens, feral or outdoor cats, and cats in multi-cat households are at higher risk of infection. Unfortunately, there is no known cure for Feline Leukemia.
A blood test can be performed in our hospital to check if a cat is infected with FeLV.
Symptoms
- Decreased appetite
- Lethargy
- Fever
- Weight loss
- Respiratory issues (coughing, sneezing, nasal or eye discharge)
- Vomiting
- Diarrhea
There are many flea and tick preventatives available today, and it can be challenging to navigate the various brands, application methods, and their pros and cons. When choosing the best option for your pet, it’s essential to consider their lifestyle, age, breed, health status, and any current medications. Since flea and tick preventatives are medications, it’s important to consult with your veterinarian before introducing a new product.
The most popular form of flea and tick prevention is topical medication, also known as "spot-on" products. These are typically applied to the base of the neck or between the shoulder blades. They work by killing fleas and ticks and can also have a repellent effect to prevent pests from attaching. Once the product has dried, your pet can swim or bathe without losing its effectiveness. However, it is crucial to wait for the medication to dry completely, and you should avoid allowing kids or other pets to interact with your pet until it has dried. Some potential side effects include itching, redness, swelling, or hair loss at the application site.
Oral medications are another option, eliminating the need for topical treatments. However, oral medications do not have a repellent effect, meaning fleas or ticks must attach to your pet before they are killed. These medications can sometimes cause stomach upset, vomiting, diarrhea, or skin reactions such as redness, itching, or hives. Additionally, some pets may refuse to take the medication, either spitting it out or avoiding it altogether.
Collars are a convenient way to protect your pet from fleas and ticks, as they don’t require application or oral medication. They contain chemicals that kill and repel fleas and ticks and are typically affordable. However, some collars may have strong odors or cause irritation to your pet’s skin. It’s also important to keep children away from the collar, as it may irritate their skin as well.
Flea and tick sprays can also be used, though they can be difficult to apply evenly for full coverage. Pets must stay dry for the spray to work, so this method isn’t ideal for pets that enjoy swimming or bathing. Be cautious when applying the spray to avoid your pet’s eyes and mouth.
Powders are another alternative, but like sprays, they can be challenging to apply evenly, and you must avoid the eyes and mouth. Possible side effects may include vomiting, diarrhea, drooling, depression, or a loss of appetite.
Shampoos can help wash away adult fleas and their eggs, but they are not long-term solutions. They work best for immediate relief from an existing flea problem and do not offer preventative care. When using flea shampoos, be sure to let the product sit for at least 15 minutes before rinsing and avoid getting it in your pet’s eyes or mouth.
Flea dips are concentrated liquids that are applied to your pet’s coat, and they need to air dry. While effective in controlling fleas and ticks, dips are not a long-term preventative solution. Dips should be applied with caution, especially on young, pregnant, or nursing pets. For safety, it’s best to have a professional administer flea dips.
When considering which flea and tick preventative is best for your pet, think about their specific needs and lifestyle. Consult with your veterinarian to find the most effective solution that provides the protection your pet requires.
- What does this product protect my pet from?
- How should I apply the product, and how frequently?
- How long will it take for the product to start working?
- What should I do if my pet appears to have a reaction?
- Does my pet need more than one product for full protection?
- If I spot a flea or tick, does it mean the product isn’t effective?
- Always consult your veterinarian before using any medication, even over-the-counter options.
- Only buy products that are EPA-registered or FDA-approved.
- Carefully read both the veterinary label and the product label on the packaging.
- Follow the instructions on the label, applying the product as directed and at the recommended intervals, unless otherwise instructed by your vet.
- Use products only for the species they are intended for. Products for dogs can be harmful to cats, so ask your vet if you're unsure.
- Make sure the product's weight range is suitable for your pet. Using a product for a lower weight can make it ineffective, while using one for a higher weight can be harmful. If you need to check your pet’s weight, all of our hospitals have scales available — no appointment necessary!
- Keep an eye on your pet for any signs of adverse reactions, especially when using a new medication. Look for signs like anxiety, skin redness or swelling, vomiting, diarrhea, excessive itching, or abnormal behavior. If you notice any reactions, contact your veterinarian and the manufacturer.
- If the flea or tick problem continues, you may need to treat your home and yard as well.
- To reduce exposure, keep your pet away from areas where fleas and ticks are likely to thrive, such as tall grass, wooded areas, and bushes.
- Perform daily tick checks, particularly after your pet has been in wooded or grassy areas. While larger ticks are easier to spot, smaller ones like deer ticks can be difficult to detect.
Heartworms are one of the deadliest parasites for both dogs and cats, and the risk of infection is high. Whether your pet is an indoor cat or a dog who loves outdoor adventures, they are all at risk for heartworm disease in the mid-Atlantic region.
Heartworms are transmitted through mosquito bites. When an infected mosquito bites your pet, it introduces larvae into the bloodstream. These larvae then travel through the soft tissue and blood vessels, ultimately reaching the heart and lungs where they mature into adult worms. Over time, adult heartworms can grow several inches long and reproduce, sending offspring into the bloodstream. When another mosquito bites the infected pet, it ingests the larvae and carries the parasite to the next host.
In dogs, heartworm disease is easier to diagnose through a blood test. The disease often results in large numbers of adult worms in the lungs and heart, which partially block blood flow and make it harder for the heart to pump blood. This leads to heart disease, shortness of breath, and coughing. As adult worms die, they cause severe inflammation in the lungs, making the symptoms worse. If left untreated, heartworm disease can result in death.
While cats are not the primary host for heartworms, studies show they are becoming infected at nearly the same rate as dogs. Infected cats suffer from lung damage as the heartworms migrate through their lungs, often dying before reaching maturity. Even so, the damage caused by the larvae’s migration can be permanent. Symptoms in cats may include coughing, shortness of breath, and even sudden death. Feline heartworm disease is often misdiagnosed as asthma, as the symptoms and radiographic findings are similar, and heartworm tests don't always detect infection in cats.
Heartworm disease in dogs can be treated with injectable medications, but the treatment is expensive, painful, and may leave permanent lung damage. Unfortunately, there is no safe treatment for heartworms in cats. The most effective approach is prevention. Both dogs and cats should receive monthly heartworm preventatives, which are inexpensive, safe, and highly effective. Even indoor pets are at risk, as mosquitoes can enter homes. Studies show that indoor cats are just as likely to be infected as outdoor ones.
In Northern Virginia, heartworm infection rates have been rising over the past decade, making it more important than ever to protect your pet. Ensure your pet is protected year-round with monthly heartworm prevention medication. For more information on heartworm disease, visit The American Heartworm Society.
Heartworm tests are blood tests used to determine if an animal is infected with heartworms. These tests can be done in-house or sent to a reference laboratory. If conducted in-house, results are often available in as little as 10 minutes.
In dogs, the heartworm test detects antigens in the blood that are produced by female heartworms. A small sample of blood is mixed with a test solution and added to a tester that contains antibodies. These antibodies bind to the heartworm antigens (proteins produced by female worms). If the antigens are present, a colored dot will appear, indicating the dog is infected. These tests are very accurate because infected dogs usually have large numbers of heartworms. However, a dog must have mature female worms in its system for the test to be positive, and since heartworms take about six months to mature, very early infections may not show up on the test.
For cats, there are two types of tests available. The first is an antigen test, similar to the one used for dogs. This test detects antigens from three or more adult female heartworms. However, most infected cats have only a few worms (typically 1-7 worms), and these may be male. If a cat has only male worms, the antigen test will likely be negative, even if the cat is infected. Therefore, while a positive antigen test in a cat confirms an infection, a negative result does not rule out heartworm disease.
The second type of test for cats is an antibody test. This test detects heartworm-specific antibodies in the bloodstream, which are produced when heartworm larvae reach the L4 stage. However, these antibodies are temporary and only last for a few months. A positive antibody test means the cat has been recently exposed to heartworms, but it doesn’t confirm the presence of adult worms. A negative test doesn’t provide much information. To improve detection, it is often recommended to run both the antigen and antibody tests, although even this combination may not detect heartworm infection in some cats.
Hookworms, named for their hook-like teeth, are one of the most dangerous intestinal parasites for dogs and cats due to their blood-feeding habits. These parasites use their sharp teeth to latch onto the intestine’s lining, where they consume large amounts of blood. A heavy hookworm infestation in puppies or kittens can lead to severe anemia, potentially resulting in death.
As hookworms move through the intestine, they can cause bleeding ulcers at each site where they attach.
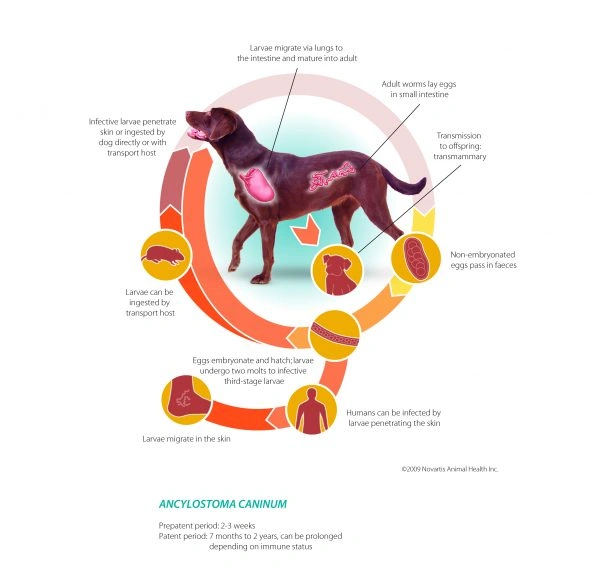
Hookworms are common in dogs and cats. The subspecies *Ancylostoma caninum* can infect puppies through the mother’s milk. Kittens are typically infected by exposure to contaminated environments. Due to their prevalence, all puppies and kittens should be routinely dewormed early in life. Hookworms are tiny and usually not visible to the naked eye, so pet owners rarely spot them in their pet's stool. Laboratory testing is needed for accurate identification.
There are several ways pets can become infected with hookworms. Puppies often get infected while nursing, as the larval worms pass through the mother's mammary tissue into the milk. Puppies, kittens, and adult animals can also ingest hookworm larvae from the environment, where the larvae hatch from eggs in the stool of infected animals. These larvae can be ingested directly or penetrate the skin of pets (and humans) who come into contact with contaminated soil. Once inside, the larvae migrate to the intestine to complete their life cycle. Additionally, dogs and cats may become infected if they eat another infected animal. Even 100% indoor pets are at risk since insects like cockroaches can carry hookworm larvae, which may then be eaten by the pet.
Hookworms are zoonotic, meaning they can also infect humans. Infection usually happens when hookworm larvae come into contact with exposed skin, often through activities like digging or walking barefoot in contaminated soil. Although humans aren’t the primary host for these worms, the larvae can cause severe skin irritation as they migrate. Thankfully, the larvae cannot complete their life cycle in humans and will die within a few weeks. The condition is called Cutaneous Larva Migrans, and treatment by a physician can help reduce symptoms. To prevent transmission, thorough hand-washing and wearing shoes in areas where infected animals may have been are crucial.
The life cycle of a hookworm takes about three to four weeks to complete.
Hookworm infection is diagnosed through fecal floatation testing. Fortunately, treatment is typically effective and straightforward. It usually involves administering a general dewormer and cleaning the environment. Indoors, vacuuming the floors and cleaning them with an all-purpose cleaner is recommended. Litter boxes and bedding should be thoroughly scrubbed and washed. All pets in the household should be dewormed simultaneously to ensure all infected animals are treated. For outdoor areas, it’s important to remove all stool, and to avoid places where many animals gather, as the soil in these areas can harbor parasite eggs for years.
Prevention is relatively simple. Most monthly heartworm preventatives for dogs and cats also protect against hookworms. These products eliminate parasites that have been contracted within the last 30 days, so it’s essential to use them consistently year-round for full protection. Pets who have not been on routine heartworm prevention can be treated with a general dewormer. Additionally, annual or bi-annual fecal floatation tests should be performed to ensure the effectiveness of the preventative medications.
For more information on hookworms, visit the Companion Animal Parasite Council’s (CAPC) webpage dedicated to hookworms.
Leptospirosis is a bacterial infection spread through the urine of infected wildlife. It is usually transmitted via contaminated water sources, such as puddles, retention ponds, and slow-moving creeks. Your veterinarian will assess you and your pet’s lifestyle to determine the risk of Leptospirosis and whether vaccination is advisable.
Often referred to as “Lepto,” the disease can lead to severe kidney and liver damage. Since Leptospirosis is zoonotic, it can be transmitted from animals to humans.
Symptoms
- Fever
- Lethargy
- Loss of appetite
- Increased thirst
- Vomiting
- Abnormal urine volume (either more or less)
- Muscle and joint pain
- Bleeding or bruising
Lyme disease is a common tick-borne infection that affects both humans and dogs. It is especially prevalent in the Northern Virginia area, and based on your pet's lifestyle, vaccination may be recommended.
Ticks typically acquire the bacteria from wildlife and transmit it to your pet when they feed. For the disease to be transmitted, the tick must remain attached for at least 48 hours. However, Lyme-carrying ticks are often very small and difficult to spot, which makes it even more crucial to keep your pet on tick preventatives and ensure they are vaccinated.
Unlike humans, dogs do not usually develop the characteristic "bull's-eye" rash. Additionally, many dogs may not show immediate symptoms, or any symptoms at all, making it challenging to detect the disease. Despite the lack of obvious signs, Lyme disease can still be present.
If a pet is positive for Lyme disease, antibiotics can be given to try to eliminate as much of the bacteria in the body. It is difficult to completely eliminate the bacteria in the body, so even with a course of antibiotics helping symptoms, a low-level infection may always be present.
Symptoms
- Some dogs may be asymptomatic and show no symptoms
- Pain
- Limping
- Lameness
- Loss of appetite
- Fever
- In severe cases, kidney and heart disease may develop
Lyme disease is the most common tick-borne illness in both dogs and humans in the United States. It is caused by the bacterium *Borrelia burgdorferi* and is transmitted through the bite of an infected tick. While many mammal species can become infected, dogs and horses are the most likely to show clinical signs of Lyme disease, while cats are naturally resistant. Lyme disease is most common along the East Coast and Great Lakes regions but is also found in other parts of the U.S.
While several tick species can harbor *Borrelia burgdorferi*, only the black-legged tick (or deer tick) and the Western black-legged tick are known to transmit the disease. Transmission occurs when a tick feeds on a host for 24-48 hours, injecting saliva containing the bacteria into the host’s bloodstream.
Most dogs infected with *Borrelia burgdorferi* are subclinical, meaning they carry the bacteria without showing symptoms. Dogs that do develop clinical signs typically exhibit fever, lameness, and general malaise. In rare cases, the bacteria may affect the kidneys, leading to protein loss and kidney failure. Lyme disease can also, though very rarely, cause heart or brain complications.
Lyme disease is treatable with antibiotics and supportive care. While treatment is usually effective in resolving symptoms, low levels of bacteria may remain in the body, and infected dogs may continue to test positive long-term. Dogs with persistent infections might show symptoms again during periods of stress or immune suppression, such as during cancer treatment.
The best way to protect your pet is to prevent Lyme disease transmission in the first place. Use a reliable tick preventative year-round to reduce your pet’s exposure. Additionally, a Lyme vaccine is available, which helps protect your dog from the Lyme bacteria if bitten by an infected tick. This vaccine is given annually after an initial two-dose booster series. In some cases, your veterinarian may also recommend antibiotic treatment after a tick bite to eliminate any bacteria before they can establish an infection.
At Caring Hands Animal Hospital, we recommend annual Lyme disease testing using our in-house Heartworm/Lyme/Ehrlichia/Anaplasmosis test. This is the most accurate way to screen for Lyme infection. If a dog tests positive, your veterinarian may recommend further testing or antibiotics. For dogs with a history of Lyme infection, we use the Lyme C6 test to measure Lyme antibody levels, helping assess the amount of *Borrelia burgdorferi* bacteria in the body. If antibody levels are rising, additional antibiotic treatment may be necessary.
Although Lyme disease is not directly transmitted from animals to humans, people can become infected through the bite of an infected tick. Currently, there is no effective Lyme vaccine for humans, so tick prevention remains the best strategy for protecting against the disease.
For more information on Lyme disease, refer to the links below:
Rabies is a fatal viral disease primarily spread by wildlife and other mammals in our area. It is zoonotic, meaning it can be transmitted from animals to humans. The disease is usually passed through the saliva of an infected animal, typically via a bite.
In Virginia, rabies vaccination is mandatory for all dogs and cats.
Symptoms
- Fever
- Seizures
- Behavioral changes (e.g., increased excitability, shyness, aggression)
- Excessive drooling
- Paralysis
- Difficulty swallowing