A Full Resource of Essential Pet Care Terms
Bordetella, commonly referred to as "Kennel Cough," is a highly contagious upper respiratory disease that affects dogs. It can be easily spread through direct contact or the air, making vaccination essential for dogs who come into contact with other dogs in various settings such as neighborhoods, boarding facilities, daycare centers, dog parks, and groomers.
Unvaccinated puppies, young dogs, and those with weakened immune systems are at a higher risk of experiencing severe symptoms.
Common Symptoms Include:
- A dry, hacking cough
- A "honking" cough
- Nasal discharge
- Decreased appetite
- Lethargy
- Fever
In 2012, a new strain of Canine Influenza emerged, originating from an existing virus. Due to its novelty, any dog exposed to it was at risk of contracting the infection. Fortunately, a vaccine has been created to safeguard dogs from the virus, and is readily accessible if necessary. It is important to note that this strain is not transmissible to humans.
Signs of Infection
- discharge from the nose or eyes
- coughing (can be productive or non-productive)
- labored breathing or increased rate
- lethargy
- vomiting
- diarrhea
- decrease in appetite
Distemper is a highly contagious viral disease that has no known cure and can affect dogs, cats, ferrets, and certain wildlife animals. The disease is spread through both direct and indirect contact.
Symptoms:
- weight loss
- lethargy
- fever
- vomiting
- diarrhea
- nasal discharge
Feline Leukemia, also known as FeLV, is a viral infection that can be transmitted between cats through saliva, feces, and during lactation. Kittens being nursed, feral or outdoor cats, and cats living in households with multiple cats are particularly vulnerable to contracting the virus. Unfortunately, there is no cure for Feline Leukemia at this time.
If there are concerns about a cat being infected with Feline Leukemia, a blood work screen can be conducted at a veterinary hospital to confirm the diagnosis.
Symptoms
- some cats can show no symptoms at all
- decrease in appetence
- lethargy
- fever
- loss of weight
- respiratory symptoms (coughing, sneezing, discharge from nose or eyes)
- vomiting
- diarrhea
With so many flea and tick preventatives available, choosing the right one for your pet can feel overwhelming. Each type has its own application method, benefits, and considerations.
Topical treatments, often called spot-on products, are applied between the shoulder blades or at the base of the neck. They spread across the pet’s body through sweat glands or bioadhesives, killing fleas and ticks and sometimes providing repellent protection. While effective, they require drying time and should not be touched until fully absorbed.
Oral medications offer a mess-free alternative, but unlike some topicals, they don’t repel parasites—fleas and ticks must bite to be eliminated. Some pets may refuse to take them, and possible side effects include vomiting, diarrhea, or skin reactions.
Collars provide long-lasting protection by releasing chemicals that kill and repel pests. They are convenient but may have a strong odor and cause skin irritation in some pets. They should also be handled with care, especially around children.
Sprays work quickly but require thorough application and may not be effective if the pet gets wet. Powders are another option, though achieving full coverage can be difficult, and ingestion can cause side effects like vomiting or drooling.
Flea shampoos wash away adult fleas and their eggs but don’t provide long-term prevention. They are useful for immediate relief but should be followed up with another preventative. Dips are highly concentrated treatments for severe infestations. They are not rinsed off and must air dry but should only be used with caution, as they are not safe for young, nursing, or pregnant pets.
Some flea and tick preventatives also protect against heartworm disease, making it important to check the product label to ensure the right coverage for your pet. Since all these treatments are medications, it’s best to consult your veterinarian before starting a new one.
- What pests does this product protect my pet from?
- How should the product be applied, and how often?
- How quickly will the product start working?
- What should I do if my pet has a reaction to the product?
- Does my pet need to use more than one product for full protection?
- If I see a flea or tick, does it mean the product isn’t effective
- Always consult your veterinarian before using any medication, even over-the-counter products.
- Purchase only EPA-registered or FDA-approved products.
- Carefully read both the veterinary and product labels on the packaging.
- Follow the label instructions exactly, applying the product as directed and at the specified intervals, unless otherwise instructed by your veterinarian.
- Use products only for the species they are intended for, as some products designed for dogs can be harmful to cats. Contact your vet if you’re unsure.
- Ensure the weight range listed on the product is suitable for your pet. Using a product for a lighter weight range may be ineffective, while one for a heavier weight range could harm your pet. You can weigh your pet at any of our hospitals without an appointment.
- Monitor your pet for any signs of an adverse reaction, especially when using a new product. Watch for symptoms like anxiety, redness, swelling, vomiting, diarrhea, excessive scratching, or unusual behavior. Notify your vet and the manufacturer if you observe any reactions.
- If the flea or tick problem persists, you may need to treat your home and yard as well.
- Minimize your pet’s exposure to fleas and ticks by avoiding areas where these pests are common, such as tall grass, wooded spots, and bushes.
- Perform a daily tick check, especially if your pet has been in wooded or grassy areas. Larger ticks are easier to spot, but smaller ones, like deer ticks, can be more difficult to detect.
Heartworms are a serious and potentially deadly parasite for both dogs and cats. Are your pets at risk? Absolutely. Whether you have an indoor-only cat or an adventurous dog, all pets in the mid-Atlantic region are vulnerable to heartworm disease.
Heartworms are transmitted through the bite of infected mosquitoes. After a mosquito feeds, the larvae enter your pet's bloodstream and travel to the heart and lungs, where they mature into adult worms. These worms can grow several inches long, causing severe damage as they reproduce and send larvae into the bloodstream, further spreading the infection.
Heartworm disease is most commonly diagnosed in dogs through a blood test. Dogs infected with heartworms often have large numbers of worms in their lungs and heart, blocking blood flow and making it harder for the heart to pump oxygen-rich blood. This can lead to heart disease, coughing, and breathing issues, and, in severe cases, can cause death. When the worms die off, they can create inflammation in the lungs, making the situation worse.
While cats are not the primary host for heartworms, they are still at risk and can be infected just as easily as dogs. Heartworms that reach the cat’s lungs often die before fully developing, but the migration process can cause permanent lung damage. Cats with heartworm disease may show signs like coughing, shortness of breath, or even sudden death, which can be mistaken for asthma. Diagnosing feline heartworm disease can be tricky, as it mimics asthma symptoms, and standard heartworm tests don’t always detect the infection in cats.
In dogs, heartworm disease can be treated with injections, but the treatment is costly, painful, and can leave permanent damage to the lungs. Unfortunately, there is no safe treatment for cats. Prevention is the key for both dogs and cats. Monthly heartworm preventatives, available through your veterinarian, are safe, affordable, and highly effective in protecting your pet. Even if your pet is indoors most of the time, mosquitoes can still enter your home, making prevention crucial year-round. Indoor cats are just as susceptible as outdoor ones, and some mosquito species that carry heartworms are active even during winter.
Heartworm infection rates in the Northern Virginia area have risen in recent years, but you can protect your pet with a simple monthly preventative. Don’t let your pet become one of the infected. Keep them safe with year-round heartworm prevention. For more information, visit The American Heartworm Society.
Heartworm tests are blood tests used to determine if an animal is infected with heartworms. The test can be done in-house or sent to a reference laboratory, with results often available in as little as 10 minutes if done in-house.
In dogs, the test works by detecting antigens of the heartworm in the blood. A few drops of blood are mixed with a test solution and poured into a tester containing antibodies that bind to heartworm antigens. A colored dot will develop if the animal is infected with heartworms. These tests are very accurate because infected dogs have a large number of heartworms in their system. However, dogs must have mature female worms in their system to test positive, as heartworms take approximately 6 months to reach maturity after infection.
There are two types of tests available for cats. One is an antigen test similar to the one used in dogs, which will turn positive if it detects antibodies of three or more adult female worms. The other test is an antibody test, which detects heartworm-specific antibodies in the cat's blood stream. A positive antibody test indicates recent heartworm infection, while a negative test may not rule out the possibility of infection.
Running both the antibody and antigen tests in cats is the best way to detect heartworm infection, but even the combination of tests may miss infection in some cats.
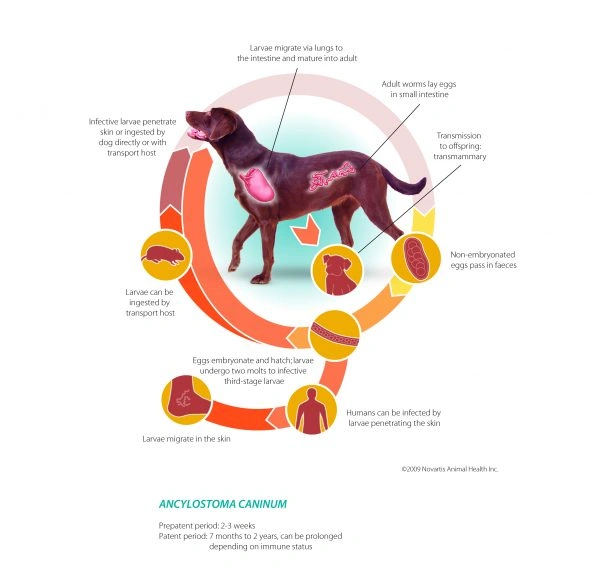
Hookworm infection is typically diagnosed through a fecal floatation test, and treatment is both effective and straightforward. Treatment usually involves administering a deworming medication and thoroughly cleaning the environment. Indoors, it's important to vacuum floors and use an all-purpose cleaner to disinfect surfaces. Litter boxes and bedding should be scrubbed and washed regularly. All pets in the household should be dewormed simultaneously to ensure that all infected animals are treated. Outdoor areas should have all stool removed, and caution should be taken when visiting places where many animals frequent, as the soil in these areas can harbor parasite eggs for years.
Fortunately, preventing hookworm infection is simple. Most monthly heartworm preventatives for both dogs and cats also protect against hookworms. These products eliminate parasites that may have been contracted in the last 30 days, so it's essential to use them consistently throughout the year for complete protection. Pets that haven't been on regular heartworm prevention can be dewormed with a general dewormer. It's also recommended to have fecal floatation tests performed annually or bi-annually to ensure that preventative medications are working effectively.
For more information about hookworms, visit the Companion Animal Parasite Council’s (CAPC) webpage.
Leptospirosis, also known as "Lepto," is a bacterial disease spread through the urine of infected wildlife. It is usually transmitted through contaminated water sources like puddles, retention ponds, and slow-moving creeks. Your vet will evaluate your pet's lifestyle to assess their risk of contracting Leptospirosis and determine if vaccination is needed. This disease can cause kidney and liver failure and is zoonotic, meaning it can be passed from animals to humans.
Symptoms:
- fever
- lethargy
- decreased appetite
- increased thirst
- vomiting
- unusual amounts of urine (larger or smaller)
- muscle and joint pain
- bleeding or brusing
Lyme disease is a common infectious disease that can be transmitted from ticks to both humans and dogs, especially in the Northern Virginia area. Depending on your and your pet's lifestyle, it may be recommended for your pet to take precautions.
Ticks usually get the bacterial disease from wildlife, and when they feed on your pet, they can pass on the disease. The tick must be attached for at least 48 hours for the disease to be transmitted to your pet. However, the ticks that carry the disease are often very small and hard to detect, so it is important to have your pet on both tick prevention and vaccination.
Dogs do not typically develop the characteristic "bulls-eye" rash from a tick bite like humans do. Since many dogs do not show immediate symptoms of Lyme disease, it can be difficult to detect. However, this does not mean that the disease is not present.
If a pet tests positive for Lyme disease, antibiotics can be given to reduce the amount of bacteria in the body. It can be challenging to completely eliminate the bacteria, so even with treatment, a low-level infection may persist.
Symptoms:
- some dogs can show no symptoms at all (asymptomatic)
- pain
- limping
- lameness
- inappetence
- fever
- in severe cases, kidney and heart disease can develop
Lyme disease is the most common tick-borne illness in both dogs and humans in the United States, caused by the Borelia Burgdorferi bacteria transmitted through the bite of an infected tick. Dogs and horses are more likely to show symptoms, while cats are generally resistant. The disease is most prevalent in the east coast and Great Lakes regions, but can be found in other areas as well.
The black-legged tick and Western black-legged tick are the main carriers, transmitting the bacteria 24-48 hours after attachment. Symptoms in dogs may include fever, lameness, and malaise, with potential complications in rare cases. Treatment involves antibiotics and supportive care, with some dogs testing positive long-term.
Prevention is key in protecting pets from Lyme disease, with tick control, vaccination, and antibiotic treatment recommended. Annual testing is advised, with additional testing and treatment if needed. Tick prevention is important for both pets and humans.
For more information on Lyme disease, please refer to the links provided below.
Rabies is a deadly viral disease that is carried by wildlife and other mammals in our region. It is a zoonotic disease, which means it can be transmitted from animals to humans. The virus is typically spread through the saliva of an infected animal, often through a bite.
In accordance with Virginia state law, all dogs and cats are required to be vaccinated against rabies.
Signs and Symptoms
- fever
- seizures
- change in behavior (over excitability, shyness, aggression)
- excessive salivation
- paralysis
- inability to swallow