The Essential Pet Care Glossary
Bordetella, often called “Kennel Cough,” is a contagious upper respiratory infection in dogs. It spreads through direct contact or airborne particles, making vaccination crucial for dogs interacting with other dogs in places like neighborhoods, boarding facilities, daycare centers, dog parks, or grooming salons.
Puppies, young dogs, and those with weakened immune systems are more susceptible and may develop severe symptoms if unvaccinated.
Common symptoms include:
- Dry, hacking cough
- "Honking" sound while coughing
- Nasal discharge
- Reduced appetite
- Lethargy
- Fever
Canine Influenza is a viral infection that originated from a mutated strain in 2012. As a new virus, it made dogs highly vulnerable to infection. A vaccine was developed for protection and is available upon request. Fortunately, this virus does not spread to humans.
Symptoms may include:
- Nasal or eye discharge
- Coughing (can be either productive or non-productive)
- Difficulty breathing or rapid breathing
- Lethargy
- Vomiting
- Diarrhea
- Decreased appetite
Distemper is a highly contagious viral disease with no cure, affecting dogs, cats, ferrets, and some wildlife species. Transmission occurs through direct and indirect contact.
Symptoms include:
- Unexplained weight loss
- Decreased energy levels
- Elevated body temperature
- Frequent vomiting
- Diarrhea
- Nasal congestion or discharge
- Dogs: DHPP protects against Distemper, Hepatitis, Parainfluenza, and Parvovirus.
- Cats: FVRCP protects against Rhinotracheitis, Calicivirus, and Panleukopenia.
Feline Leukemia (FeLV) is a viral infection that spreads between cats through saliva, feces, and nursing. Kittens, outdoor cats, and those in multi-cat households face a higher risk of infection. There is currently no cure for FeLV.
A blood test can determine whether a cat is infected.
Symptoms may include:
- Decreased appetite
- Lethargy
- Fever
- Weight loss
- Respiratory issues (coughing, sneezing, nasal or eye discharge)
- Vomiting
- Diarrhea
Choosing the right flea and tick preventative for your pet can be challenging due to the variety of options available. It is crucial to consider factors such as your pet's lifestyle, age, breed, health condition, and current medications when making a decision. Before introducing a new product, it is essential to consult with your veterinarian as these are medications.
Topical medications, also known as "spot-on" treatments, are applied to the base of the neck or between the shoulder blades. These products not only kill fleas and ticks but also repel future infestations. It is important to ensure the product dries completely before allowing interaction with children or other pets, as possible side effects may include itching, redness, swelling, or hair loss at the application site.
Oral medications provide an alternative to topical treatments but do not offer a repellent effect. Some oral medications may cause side effects such as vomiting, diarrhea, or skin irritation.
Collars are a convenient option for killing and repelling fleas and ticks, although some may have strong odors or cause skin irritation. It is crucial to prevent children from touching the collar to avoid irritation.
Flea and tick sprays can be effective but may be challenging to apply evenly. Pets must remain dry for the spray to work, making this method less ideal for pets that enjoy swimming.
Powders, like sprays, are another option but can be difficult to apply evenly and may cause side effects if ingested.
Shampoos provide immediate relief by washing away adult fleas and their eggs but do not offer long-term protection. They are best suited for short-term control.
Flea dips involve applying a concentrated liquid to your pet's coat and allowing it to air dry. While effective, dips are not a long-term solution and should be applied with caution, especially on young, pregnant, or nursing pets.
When choosing a preventative, it is important to consider your pet's individual needs and consult with your veterinarian to ensure the most effective protection.
- What does this product protect my pet from?
- How frequently should I apply or administer the product?
- How long does it take for the product to become effective?
- What should I do if my pet has an adverse reaction?
- Does my pet require multiple products for full protection?
- If I spot a flea or tick, does it mean the product isn’t effective?
- Consult Your Veterinarian: Always speak with your veterinarian before starting any new medication, including over-the-counter options. They can recommend the most suitable product for your pet based on their health, weight, and lifestyle.
- Choose EPA-Registered or FDA-Approved Products: Only use products that are approved by the EPA (Environmental Protection Agency) or FDA (Food and Drug Administration). These products undergo rigorous testing to ensure they are both safe and effective.
- Read and Follow Label Instructions Carefully: Carefully read the product label and any additional instructions provided by your veterinarian. Apply or administer the product exactly as directed and at the recommended intervals to maintain effectiveness.
- Use Products Designed for Your Pet’s Species: Never use a product intended for one species on another. For example, flea and tick preventatives designed for dogs can be harmful or even fatal to cats. If you are unsure about a product’s suitability, consult your veterinarian.
- Ensure Correct Dosage for Your Pet’s Weight: Make sure the product you choose matches your pet’s weight range. Using a product intended for a lower weight can make it ineffective, while using one for a higher weight may cause harmful side effects. If you’re unsure of your pet’s weight, all of our hospitals have scales available for a quick check — no appointment necessary.
- Monitor Your Pet for Adverse Reactions: Pay close attention to your pet after applying or administering a new flea or tick preventative. Watch for signs of adverse reactions such as skin redness, swelling, itching, vomiting, diarrhea, excessive scratching, or changes in behavior. If you notice any concerning symptoms, contact your veterinarian immediately and report the reaction to the manufacturer.
- Treat Your Home and Yard if Necessary: If the flea or tick infestation persists despite using preventatives, you may need to address the environment by treating your home and yard. Fleas and ticks can thrive in carpets, bedding, and outdoor areas, so comprehensive treatment may be required.
- Limit Exposure to Flea and Tick Habitats: Minimize your pet’s exposure to areas where fleas and ticks are likely to thrive, such as tall grass, wooded areas, and bushes. Fleas and ticks often hide in these areas and can easily latch onto your pet.
- Perform Daily Tick Checks: After your pet spends time outdoors, especially in wooded or grassy areas, perform a thorough tick check. While larger ticks are easy to spot, smaller ones like deer ticks can be difficult to detect. Pay close attention to areas like the ears, neck, underarms, and between the toes.
Heartworms pose a significant threat to both dogs and cats, with a high risk of infection in Arlington, VA. These parasites are transmitted through mosquito bites, introducing larvae into the bloodstream that eventually mature into adult worms in the heart and lungs. In dogs, heartworm disease can lead to heart issues, difficulty breathing, and coughing, while in cats, it can cause lung damage and even sudden death.
Treatment for heartworm disease in dogs is available but costly and painful, with potential permanent lung damage. Unfortunately, there is no safe treatment for infected cats. Prevention is key for both pets, with monthly heartworm preventatives being highly effective and affordable. Even indoor pets are at risk, as mosquitoes can enter homes.
In Arlington, VA, heartworm infection rates have been on the rise, emphasizing the importance of protecting your pet year-round. For more information on heartworm disease, visit The American Heartworm Society.
Heartworm tests can determine if an animal has been infected with heartworms. These tests can be done on-site for quick results or sent to a lab for further analysis.
In dogs, the test looks for antigens produced by female heartworms in the blood. A blood sample is mixed with a solution and applied to a device with antibodies. If heartworm antigens are present, a colored dot will appear, confirming the infection. These tests are reliable because infected dogs usually have many worms, but it may take six months for mature female worms to develop, so early infections could be missed.
For cats, there are two types of tests available. The first is an antigen test like the one for dogs, which detects antigens from at least three adult female heartworms. However, most infected cats have only a few worms, and if they are male, the test may give a false negative result.
The second test for cats is an antibody test, which identifies heartworm-specific antibodies produced when larvae reach the L4 stage. These antibodies are temporary and may not last long. A positive result means the cat was recently exposed to heartworms, but it doesn't guarantee the presence of adult worms. A negative result also doesn't rule out infection. To improve accuracy, veterinarians often recommend both antigen and antibody tests, but even this may not always detect heartworm infections in cats.
Hookworms are dangerous intestinal parasites for dogs and cats because they feed on blood by latching onto the intestinal lining with their hook-like teeth. Severe infestations can lead to anemia, which can be fatal if not treated promptly. These parasites leave behind bleeding ulcers as they move through the intestines.
Hookworm infestations are common in dogs and cats, with puppies and kittens at higher risk. It is important to deworm pets early in life since hookworms can be passed from mother to offspring or contracted from contaminated environments. Laboratory testing is necessary for accurate diagnosis due to the small size of the parasites.
Pets can become infected with hookworms through various means, including nursing, ingesting larvae from contaminated environments, or consuming infected animals. Even indoor pets are at risk, as insects like cockroaches can carry hookworm larvae. Humans can also be infected, usually through contact with contaminated soil, but the larvae cannot complete their life cycle in humans and will die within a few weeks.
Preventative measures, such as wearing shoes and practicing good hygiene in areas where infected animals may have been, can help reduce the risk of transmission to both pets and humans. Cutaneous Larva Migrans, caused by hookworm larvae migrating through the skin, can be treated by a physician to alleviate symptoms.
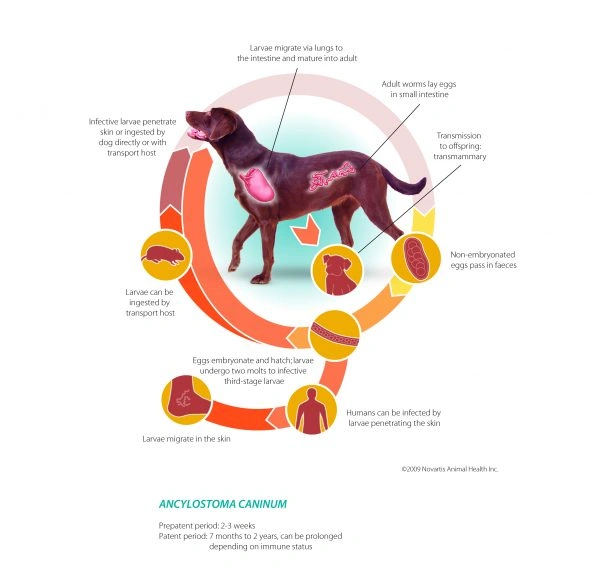
Hookworm infections are diagnosed through fecal flotation tests. Treatment involves giving a broad-spectrum dewormer and thoroughly cleaning the pet’s environment. This includes vacuuming and washing floors, scrubbing litter boxes, and laundering bedding indoors. Outdoors, it is important to remove all stool and avoid areas where many animals gather, as the soil in these locations can harbor parasite eggs for years.
Prevention is easy and effective. Most monthly heartworm preventatives for dogs and cats also protect against hookworms. These products eliminate parasites acquired in the last 30 days, so year-round use is necessary for continued protection. For pets not on routine heartworm prevention, a general dewormer can clear any existing infections. Routine fecal flotation tests should be done annually or bi-annually to confirm the effectiveness of preventive measures.
Leptospirosis is a bacterial infection that is mainly spread through the urine of infected wildlife. Pets can become infected by coming into contact with contaminated water sources, such as puddles, retention ponds, or slow-moving streams. Your veterinarian will evaluate your pet's lifestyle to determine the risk of Leptospirosis and whether vaccination is necessary.
Also known as "Lepto," this disease can cause serious kidney and liver damage. Because Leptospirosis is zoonotic, it can be transmitted from animals to humans.
Symptoms of Leptospirosis may include:
- Fever
- Lethargy
- Loss of appetite
- Increased thirst
- Vomiting
- Abnormal urine volume (either more or less)
- Muscle and joint pain
- Bleeding or bruising
Lyme disease is a common tick-borne illness that affects both dogs and humans, particularly in Northern Virginia. Your veterinarian may recommend vaccination based on your pet's lifestyle.
Ticks can transmit the bacteria to your pet while feeding, but they must be attached for at least 48 hours for transmission to occur. Since Lyme-carrying ticks are often small and hard to spot, it's important to use a reliable tick preventative and ensure your pet is vaccinated.
Dogs rarely show the classic "bull's-eye" rash seen in humans when infected with Lyme disease. Many dogs may not show immediate symptoms, making early detection challenging. Even without symptoms, Lyme disease can still be present and pose a threat to your pet's health.
If your pet tests positive for Lyme disease, antibiotics can help reduce the bacterial load. However, completely eliminating the bacteria is challenging, and a low-level infection may persist even after treatment.
Symptoms:
- Some dogs may be asymptomatic and show no symptoms
- Pain
- Limping
- Lameness
- Loss of appetite
- Fever
- In severe cases, kidney and heart disease may develop
Lyme disease, caused by the bacterium Borrelia burgdorferi, is the most common tick-borne illness affecting dogs and humans in the United States. It is primarily spread through the bite of an infected tick. Dogs and horses are more likely to show symptoms, while cats are usually resistant. Lyme disease is most prevalent on the East Coast and Great Lakes regions but can occur in other parts of the country.
The black-legged tick (deer tick) and Western black-legged tick are known to transmit Borrelia burgdorferi. Transmission occurs when an infected tick remains attached to the host for 24-48 hours, injecting bacteria into the bloodstream.
Most dogs with Borrelia burgdorferi show no symptoms, but when they do occur, they may include fever, lameness, and lethargy. In severe cases, the bacteria can affect the kidneys, leading to kidney failure. Heart or brain complications are rare.
Treatment involves antibiotics and supportive care. However, low levels of bacteria may remain in the body, causing recurrent symptoms during times of stress or immune suppression.
Prevention is key in avoiding Lyme disease. Using tick preventatives year-round can reduce your pet's risk. A Lyme vaccine is available for dogs to protect against infection. Annual testing for Lyme disease is recommended, and additional testing or antibiotics may be necessary if a dog tests positive.
While Lyme disease cannot be transmitted directly from animals to humans, humans can get infected through tick bites. Tick prevention is crucial since there is no vaccine available for humans.
For more information on Lyme disease, please visit the provided resources.
Rabies is a deadly viral illness that mainly spreads through wildlife and other mammals in the area. It is zoonotic, which means it can be transmitted from animals to humans, often through the saliva of an infected animal, usually through a bite.
In Virginia, it is required for all dogs and cats to receive rabies vaccinations.
Common symptoms of rabies may include:
- Fever
- Seizures
- Behavioral changes (e.g., increased excitability, shyness, aggression)
- Excessive drooling
- Paralysis
- Difficulty swallowing